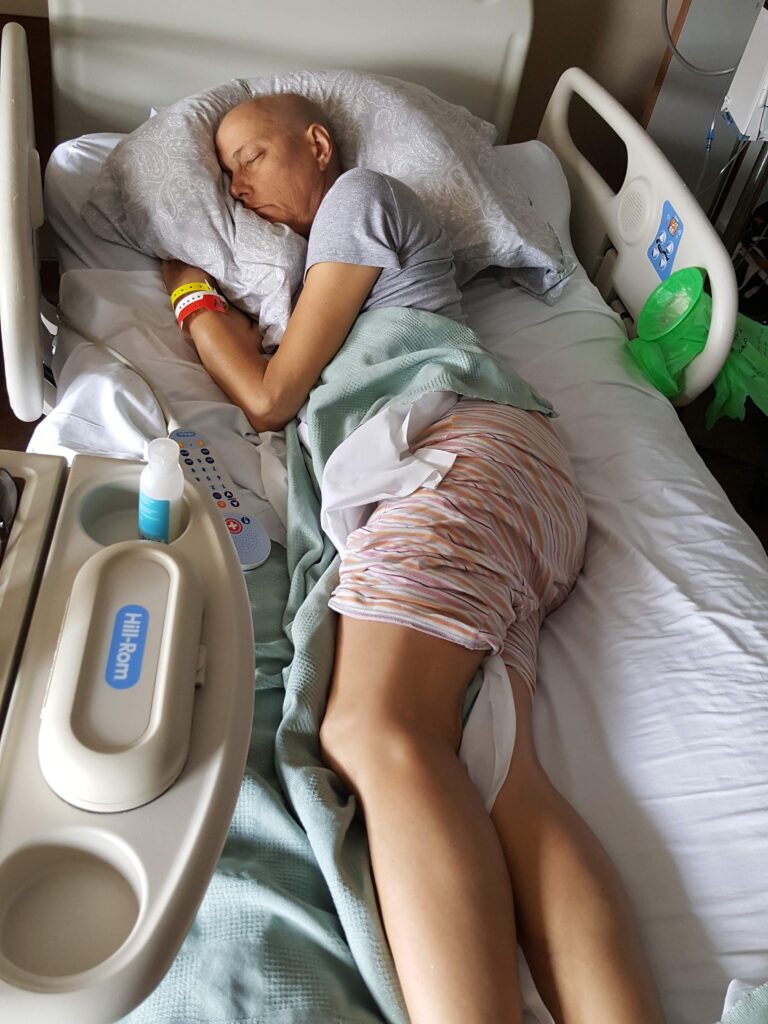
Pam’s Story of Living with AML (September)
Written by Pam Wilson
When I set about to tell my cancer story, I just had a hard time summing it all up so I just assumed I was never going to be able to write well enough to be called a writer. For some reason that has always been important to me. I want to convey to others how I feel. While in stall mode, I picked up my journal. To this day, I cannot actually remember how I wrote it. I am going to give you a couple of these entries. I figure most people like to hear the raw truth, no editing, no one judging you. I want you to know the truth of living with acute myeloid leukemia (AML). I don’t say surviving AML as if it’s over. It will never be over. This is a big, huge, scary, and mean cancer. To that end, I want to share what I penned in my most vulnerable moments.
“And so, with the sunshine and the great bursts of leaves growing on the trees, just as things grow in fast movies, I had that familiar conviction that life was beginning over again with the fall. “ -F. Scott Fitzgerald
I have now been transplanted, which was somewhat uneventful after all the other grueling things I have been through. It basically was hanging a bag of my sister’s bone marrow to be infused into my veins. I was completely unprepared for what would come next.
As you may suspect, my journaling came to a screeching halt as I was too sick to sit up most days. My worst day was day six. The goal, for now, is to make it to day 100 – the day they say you are out of the woods of imminent death. That is both scary and very short. Being isolated and quarantined to a separate bathroom and bedroom made time go so slowly – it felt like an eternity to me. My family put a small fridge in my room, set up Roku, and gave me a large cowbell to call for help when I needed it.
It is mind-boggling how much you are required to cope with. I spent the next few weeks in the hospital, getting sick in one form or another. I could not keep anything down. At times, I could not swallow my saliva and needed a suction machine. This did a real number on my daughter. She hated the sound and the constant reminder of how sick I was.
My goal was to sit up daily, walk, and try to eat. Protein was very important, but all I wanted was ice cups. Walking even became daunting. I needed three people to help walk me. Two pushed a pole loaded with boxes and IV lines, one or both attached to my port and my tri fusion catheter. The nurse would then guide me and keep me from falling. I did manage to sit up in a chair most days. By far, eating was the most difficult thing I faced. Whatever I put in my mouth came out, and wearing a diaper was not a fashion statement but a reality.
This went on for 29 days! Each day was excruciating, lonely, scary, maddening, and relentless.
By now, my family had begun tag teaming their visits so they could have some time to themselves. I felt horrible pulling them from their lives and routines. We all had no choice, so I knew I was not alone, but it bothered me to be so dependent on them.
Someone brought me a book to write a highlight every day. Brilliant as it kept me positive. It did not get a daily entry, but on good days, I celebrated small victories like I sat up twice and my food stayed down. I also wrote down how grateful I was for the nurses and physicians, my family near and far, my occasional visitor, and my ice cream cups that soothed my throat. I was wasting away, and it was hard to see my body so ravished. I eventually received liquid feedings through my IV.
When I was able to journal, I wrote about the side effects I was feeling. One particular drug called tacrolimus made me shake so bad that I could not get any utensil to my mouth without losing the contents on my clothes. Finger foods was where I was at.
This is what I penned about tacrolimus:
This shaking keeps me steady. I should know.
It has become my new norm. I can count on it to make me appreciate when I am still. It is a reminder that I am not in control. I have to learn to work with each side effect like it is my friend. What good is it? It slows me down; it makes me seek help. Why do I fear this so? It has made me change my pace, my trajectory, and my desire to go things alone.
This shaking makes me steady. I should know as I am becoming someone I do not know.
Probably the scariest moment was when I had a code blue.
The sound I hear is a steady beep. It yells in urgency, but often gets a slow reaction from the nursing staff, throwing me into a panic when they don’t automatically appear as I imagined. To me, it says, “DANGER, DANGER.” My mind races, I could die. I push the call button to hurry their arrival. They come in calmy and give me cortisol. I must now attempt to get back to sleep to make the night pass more quickly.
The alarm goes off again, waking me from my safety net of dreams. The panic rises in me again. I check all the lines attached to me, wondering what is wrong this time. I try to console my fears while I wait.
I now awaken to a team around me, pushing, prodding, pulling to get me to breathe again. I am being held by my arms while they try to retrieve blood gases. They tell me they took 15 liters of water from my lungs. I have them call my husband because I now fear I will die alone. I want to tell him my last wishes, that I love him and to take care of my children. They eventually give me a sedative, and I drift off, and my husband goes home to sleep.
Oh, the sound of that machine. It will forever take me back to a sense of fear and pain. Then, I think hearing that sound is proof I am still alive. I must talk myself down and embrace the rhythm that is my sense of still being alive.
So, this is what September was like. I am glad I am still here to tell you about it.